
Well, it’s back. I just finished a week in the ICU and COVID has come back with a vengeance. Our numbers tripled over just a couple weeks, faster than at any other time in the pandemic. We went from having no patients in the ICU to having a third of our ICU patients having COVID-19. Outside the hospital I started getting calls from neighbors and friends with questions about isolation and quarantine and reports from local testing sites of lines out the door around the building. In short, it started to feel more like December 2020 than December 2021. It was déjà vu all over again and, just like every other time, it was exhausting physically and emotionally.
With the rapid rise in Omicron, things started to sound very familiar to prior waves. Everyone was bracing for more restrictive mitigation strategies when the CDC issued a statement 12/27 that seemed out of step with the frightening rise in case numbers. They were more lenient this time.
I have always felt that sorting through the CDC website is the Internet equivalent of waiting in line at the DMV minus the excessive fluorescent lighting. My goal, as always, is to help simplify the confusing swarm of sometimes contradictory information and clarify the reasons behind the recommendations. I’ll start by explaining the recommendations first and then I’ll try to explain the rationale. We’ll end with a bit of optimism.
The easiest way to understand the recommendations is to break them down into two categories – isolation and quarantine – and two groups – well-vaccinated and under-vaccinated. Remember, ‘isolation’ is for someone who has tested positive for COVID-19 while ‘quarantine’ is for someone who has been exposed but has not acquired the infection.
If you tested positive for COVID-19
If you test positive the recommendations are the same regardless of vaccination status. Everybody who tests positive is recommended to isolate for five days regardless of symptoms or vaccination status. The clock starts from symptom onset or from your test date if you did not have symptoms. If you have no symptoms or your symptoms are resolving on day five you can end your isolation. It is important to note that if you are still having fevers, even if your symptoms are improving, you should continue to isolate until your temperature comes down. Fevers are a sign of high contagiousness. After leaving isolation you should be strict about mask wearing for an additional five days. When they say ‘wear a mask’ this, of course, means no chin diapers or gaiters. Remember, there is still a higher chance that you could infect someone else during this period than under normal conditions.
Everybody who tests positive is recommended to isolate for five days regardless of symptoms or vaccination status.
You were exposed to somebody who tested positive.
He is where things get a little more confusing because vaccination status comes into play. I think it is best to break down this group into 2 categories, well-vaccinated and under-vaccinated. The under-vaccinated group includes those who have made the unfortunate decision to remain unvaccinated.
Well-vaccinated:
There are 3 categories in this group:
- Those with a booster.
- Those who had the Pfizer or Moderna vaccine less than 6 months prior.
- Those who had the Johnson & Johnson vaccine less than 2 months prior.
If you are in this category and you have been exposed to someone with COVID-19 you do not need to quarantine but should wear a mask for 10 days and, if possible, get a test on day five. Of course, if you develop symptoms at any time during this period you should get tested. If you test positive your clock starts for your isolation as delineated above.
If you are well-vaccinated and you have been exposed to someone with COVID-19 you do not need to quarantine but should wear a mask for 10 days
Under-vaccinated:
If you do not fall into the above 3 categories from the well-vaccinated group you are under-vaccinated. If you are in this category and have been exposed to someone with COVID-19, you should quarantine for five days and continue to wear a mask for five additional days. If you are unable to quarantine you should be very strict about mask-wearing for 10 days. You should test on day five if possible
Omicron is more contagious but causes less severe disease
At this point, you may be asking, why the change? We have all been used to the standard isolation and quarantine guidelines which have had only one major change in almost 2 years, why the change and why now?
To answer this question, it is important to recognize that every viral variant is unique. Just because Omicron is a variant of SARS-CoV-2 does not mean that it will behave like prior variants. Omicron COVID-19 is a different disease than delta COVID-19, alpha COVID-19, or the OG virus.
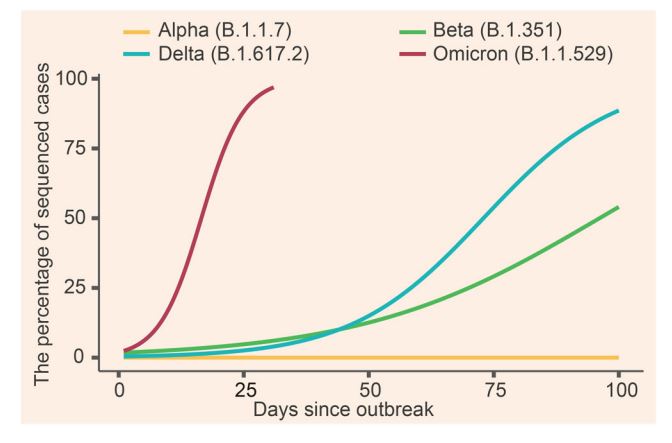
Omicron became a variant of concern in late November. It contained 3-5 times as many mutations as prior strains and spread at a speed that was alarming to everyone. Data from South Africa’s largest health insurer confirmed that it was far more contagious than prior strains. The same data also showed that it was better at evading the immune response. People with prior infection from previous strains and those who were vaccinated were much more likely to get reinfected. It was also spreading very rapidly in areas that had achieved herd immunity from delta.
It was clear early on that Omicron was more contagious, but more contagious does not always mean more severe. Research subsequently showed that Omicron multiplies 70 times faster in the upper respiratory tract (i.e. the nose and mouth) but is 10 times less efficient at replicating in the lower respiratory tract. Pneumonia is a condition of the lower respiratory tract and was the main cause of death from COVID-19 so a variant that multiplies more in the upper respiratory tract and less in the lower respiratory tract would cause more rapid spread but less severe disease. This is what is being seen in the data. It is also what my colleagues and I are seeing in the hospital. Even though the case numbers have spiked dramatically and we are seeing more ICU cases the number of ICU cases relative to the number of admissions is less. A year ago if we were to have this many hospitalizations we would have had many more ICU patients than we do now.
This does not mean that people are not dying, they are, just at a lower rate relative to prior strains. Do not forget, just because somebody does not die does not mean they are not permanently altered for the worse as a result of their infection. None of our ICU patients come out of the ICU the same people they were before they got sick.
Another thing we are seeing is that this is now a pandemic of the unvaccinated. The research shows that vaccine effectiveness against infection for two doses of an mRNA vaccine is approximately 35%. A COVID-19 vaccine booster dose restores vaccine effectiveness against infection to 75%. All levels of vaccination significantly decrease the risk of severe disease, hospitalization, and death from Omicron even if they don’t completely prevent infection. All but one ICU patient we have with COVID is unvaccinated.
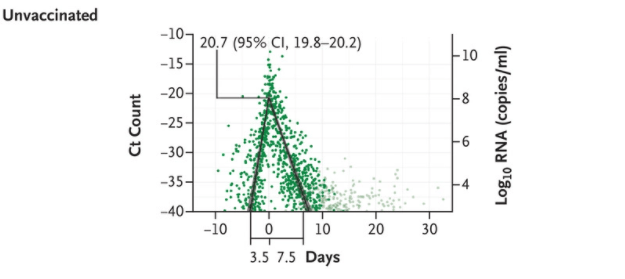
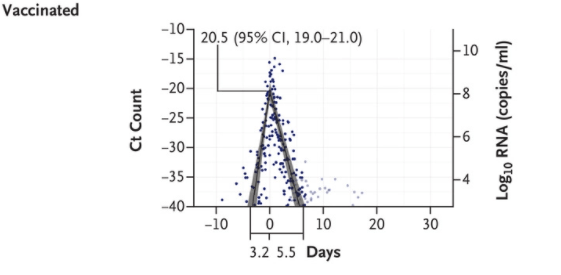
People who are vaccinated clear the virus much faster than the unvaccinated
On December 23 the New England Journal of Medicine published research showing that vaccinated individuals clear the virus significantly faster than the unvaccinated and are therefore are contagious for a shorter time.
One other important factor
Since Omicron is more contagious and the vaccines are less effective at preventing infection numerous healthcare workers have been out sick. There is now a staffing crisis in hospitals. This could lead to more morbidity and mortality than the virus itself.
All of that put together:
When we put all of the above information together the reason for the change in the CDC recommendations should be clear.
- Omicron is significantly more contagious but causes less severe disease.
- Two doses of the Pfizer and Moderna vaccines are insufficient to prevent infection but still prevent severe disease.
- Three doses do a good job of preventing infection and a great job of preventing severe disease.
- Vaccinated individuals shed the virus for a shorter time than the unvaccinated.
- If a change was not made to the recommendations there could be a crisis in hospitals caused by a shortage of hospital staff.
Hopefully this makes it clear why the isolation and quarantine times were made shorter and why there are different recommendations for the vaccinated and unvaccinated.
Reason for optimism
Now for the good news. There is good reason to believe that this may be the final wave of COVID-19.
First, even though each new variant may evade the antibody response to some extent, infections leaves a remnant of protection from other segments of the immune response. These confer some protection from future strains and are cumulative. This would be true about immunity achieved from both natural infection and vaccines.

Second, as we see with Omicron, it is to a virus’s evolutionary advantage to become more contagious but cause less severe disease. If the virus makes people very sick they lie in bed instead of spreading the germ around. A virus likes to get around and killing or incapacitating its host is a poor strategy. This is also why most viral pandemics last between 2.5 to 3.5 years. Some people believe this is how the 1918 flu pandemic ended. A new strain mutated that was more contagious but less severe. This strain then led to widespread immunity to the more severe strains to a level that made infection significantly less fatal.
As we approach the new year we should all be optimistic that 2022 will be far better than 2021, at least as far as the pandemic is concerned. I know that this is what they said last year, but this time is different. This time I believe it.
I love how your blog takes something confusing and makes it understandable to the masses! Thanks!
One thing I see that the CDC—and you—do not address is immunity from previous infection. Is this because there’s less data on this? Or reflects the CDC pushing an agenda toward vaccination? If someone had COVID during the delta wave and did not receive a booster, where would that person’s level of risk fall?
LikeLike
Data from South Africa showed that the booster plus prior infection was effective at preventing omicron. 2 doses was shown to lack significant efficacy. I don’t know if there is data comparing 2 shots plus prior infection to 3 shots plus prior infection. I personally want all the protection I can get. I have no fear of vaccines. I’ve been getting them for 44 years without any problem.
As to the CDC pushing an agenda, I have known many scientists who worked at the CDC (I went to medical school one block up the road). All of them had the only agenda of improving public health. They did so at great financial cost, turning down much higher paying jobs. This is not to say they are perfect; to expect perfection under the circumstances they work is unreasonable. If it seems like they have an agenda pushing vaccines it is because this is what they truly believe will improve public health. I do get somewhat frustrated (as evidenced by the length of this response) with those (not you) in the public who vilify these people while accepting the word of politicians on social media influencers instead.
LikeLike
Again, thank you Dr Grove for all you do..
Sandy
LikeLike
Thank you so much for this clear and optimistic post! One angle that you don’t mention, and that I haven’t seen mentioned in many of the articles I’ve read on Omicron, is what you’ve seen and read about the effect on immuno-compromised and otherwise high-risk people who are fully vaccinated (including booster). Have you seen any data or experienced anything anecdotally on the severity and impact on those groups of individuals?
LikeLike
Sorry but I haven’t.
LikeLike