It is not that I am a masochist, I’m just a bit impulsive. There I was again, in the same conference room I had been two times before back in December and January, lifting up my sleeve to get vaccinated against COVID-19. On one side of the room was a nurse with smiling eyes cheerfully administering my 3rd dose of the Pfizer vaccine just like the previous two times. This time, however, there was another nurse a few tables over willing to give me a flu shot. Why would I want to get both vaccines and a double shot of that crummy post-vaccine feeling? The answer is simple. I need to get them done at work otherwise I have to somehow prove to the HR department that I was vaccinated elsewhere. This involves emailing forms to nameless and faceless mailboxes, hoping there is someone checking at the other end. The pain of dealing with the bureaucracy of a multi-billion dollar healthcare corporation is far greater than the combined pain of both vaccinations. The real question is, was it the right thing for me to get the booster, and should you get yours as well. It turns out this is quite a difficult question to answer.
In mid-August, the Food and Drug Administration (FDA) amended the emergency use authorizations for Pfizer-BioNTech and Moderna to allow a third dose of their COVID-19 vaccines for certain populations. Then, in September, the FDA authorized—and the Centers for Disease Control and Prevention (CDC) recommended—a booster of the Pfizer-BioNTech vaccine for people 65 and up, residents of long-term care settings, and people 50 to 64 with underlying medical issues; the booster is recommended at least six months after receiving the second dose of the primary series. Additionally, the CDC says a booster dose of Pfizer-BioNTech may be recommended for people 18 to 49 with underlying medical issues, and for people 18 to 64 whose profession may put them at higher risk of exposure to COVID-19. That last group of people can include health care workers, teachers, and others. What is the evidence for these recommendations?
The Evidence
The idea of a booster is not new or crazy. It is normal for antibodies to viruses to decrease over time and most vaccines require a booster at one point. Most of us received additional shots spaced at different time intervals for illnesses such as chickenpox, tetanus, diphtheria, mumps, measles, and rubella among others. Vaccination produces an initial surge in the number of immune cells and antibodies which then slowly drops. This leaves behind a small pool of long-lasting ‘memory’ cells that patrol the body for future infections by that particular bug. Boosters cause antibody-making B cells to multiply, elevating the levels of antibodies. After a booster, the number of memory B cells will be larger and better prepared to respond to reinfection. Further, boosters promote a process called “affinity” maturation where the B cells that have been triggered by the vaccine are mutated in a way that makes the antibodies they produce bind to pathogens more strongly. For this reason, it was believed the people would benefit from a booster shot of the COVID vaccines as well. There is evidence that third doses of vaccines developed by Moderna, Pfizer–BioNTech, Oxford–AstraZeneca and Sinovac prompted a spike in levels of infection-blocking ‘neutralizing’ antibodies when administered several months after the second dose.
Most experts expected vaccine effectiveness to wane, at least measured by antibody responses, and this has happened with SARS-CoV2 as well. Then came Delta and vaccine effectiveness took another hit and the world took notice. Israel had been the earliest to vaccinate a large portion of its citizens and was hit hard by Delta with a rapid rise in infections with over half of hospitalized patients being vaccinated. The Israeli Ministry of Health estimated that vaccine protection against both infection and disease had dropped from above 90% in the early months of its program to around 40% by late June. Data also showed that individuals who were vaccinated earlier had less protection against Delta with the effect of waning seen after about 6 months. What was interesting was that the percentage of breakthrough cases was far higher than in other countries with similar vaccination rates like Great Britain the breakthrough rates were much lower.
Why did the vaccine not work as well in Israel? It wasn’t the sunshine or the falafel. The reason is believed to be in large part related to when the vaccine was given and how it was spaced apart. Israel gave its vaccines very early compared to other countries so there was more time for effectiveness to wane. Additionally, they gave the Pfizer vaccine which was studied with doses given 3 weeks apart. This is highly unusual for vaccines which typically have a several-month delay between doses to maximize efficacy. The immune response must fully develop and transition to the memory phase for additional doses to get the maximal effect. The time crunch created by the severity of the pandemic caused the dosing schedule to be shortened. So Israel gave the vaccine early with doses spaced 3 weeks apart.
All this pointed to waning immunity and decreased effectiveness against Delta being the cause of the surge in infections and serious illness.
This was not the case in other countries. In the early days of the vaccine rollout, countries with more limited supply (e.g. Canada and the UK) were forced to space out their two doses by 8-12 weeks to get as many first doses in as possible before moving on to the second dose. It is hypothesized that the better response in those countries may be the result of the delayed second dose producing a longer and more durable response. As an aside, this is one reason why the Moderna vaccine, which had a 4 week instead of 3-week schedule, may be more effective than Pfizer. So these countries gave their doses later and more spaced apart. All this pointed to waning immunity and decreased effectiveness against Delta being the cause of the surge in infections and serious illness.
At the same time, there was evidence that both the Pfizer and Moderna boosters demonstrated broad antibody boosting after a third dose and better antibody responses are associated with a lower risk of severe infection. So we combine waning immunity and decreased effectiveness against a new variant with evidence that third doses effectively boost immune responses.
A preliminary study of 149,144 people over 60 showing that a Pfizer booster shot reduced the chances of infection by 86% and reduced the chance of severe infection by 92%. All of this prompted Israel to authorize a booster shot for citizens over 16, starting with the most vulnerable. Fortunately for the world, they published the data from those over aged 60 comparing those with the booster to those without. These were the results:
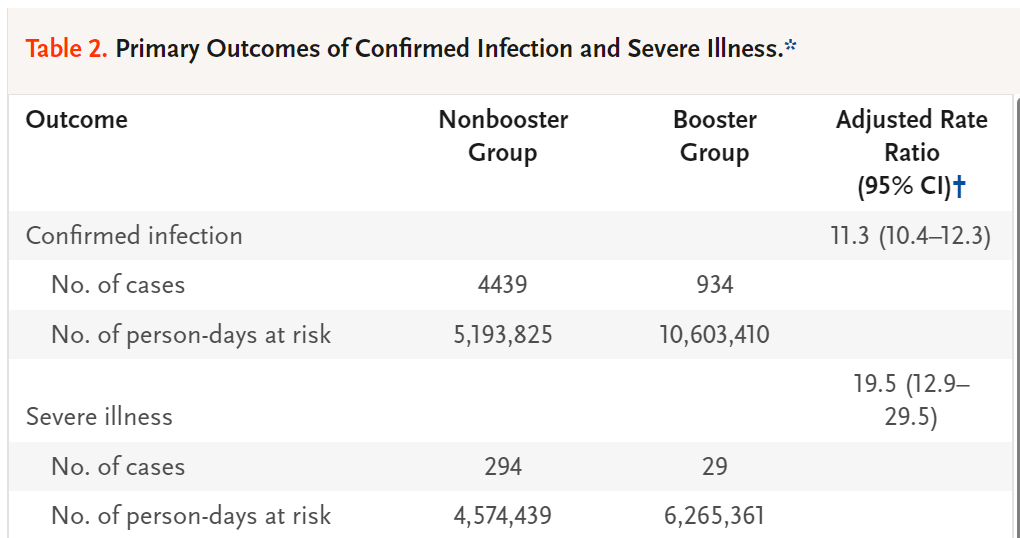
You can see from these numbers that the risk of infection is 11.3 times higher and the risk of severe infection is 19.5 times higher in the group that did not get the booster. They estimated vaccine efficacy of 95% with the third dose. The booster worked in this population and probably did as well in younger individuals as well.
The Controversy
Based on the above evidence the FDA gave the green light to Americans over 65 and to those between 18 and 64 with a specific list of immunocompromising conditions to get a Pfizer booster and just approved a half dose Moderna booster as well. They also approved a group of healthy people aged 18-64 “whose frequent institutional or occupational exposure” to the virus puts them at high risk. The CDC adopted these recommendations. The Biden administration had endorsed boosters for all over 16.
There is evidence for those who have received organ transplants and are on immune-suppressing anti-rejection medications that the booster improves the vaccine response. This could be extrapolated to those on other similar medications, like chemotherapy or autoimmune medications, but what about those with chronic lung and heart disease or those with cancers not on those medications?
That is the data for those over 60 and the severely immunocompromised, but what about everyone else? What about other forms of immunocompromise? What about younger more healthy individuals? What about those with high exposure like front-line health care workers?
The booster is likely to improve immunity in younger and healthier individuals as well but their risk of severe disease is extremely low after they are fully vaccinated the first time. So, even though the booster will improve their immunity, it is not necessary and those doses can be sent to those in the world who are yet to get their first dose.
I do not envy those who have recommendations based on this information but I know that those who are critical of the decisions have no idea what goes into making them.
The other side of the equation is important as well. The safety of these vaccines is remarkable. As of October 14th, 3,777,779,372 people have received at least one dose and there have been no reports of serious side effects in numbers that would be even close to a cause for concern.
The question of whether or not to give a booster is, of course, more complicated than just a matter of risk vs benefit. There are the problems of limited data, questions of timing, issues of global epidemiology, and geopolitics. The consequences of being wrong could be more death, more shutdowns, and more economic downturn. I do not envy those who have to make recommendations based on this information but I know that those who are critical of the decisions have no idea what goes into making them.
For noble and understandable reasons, the CDC, the FDA, and the White House are erring on the side of safety for the populations they serve. Immunity seems to wane, the Delta is killing thousands a day, there is evidence that a booster helps, and the side effects of the vaccine are negligible.
The next variant to cause us pain could be brewing in an underdeveloped unvaccinated population right now.
How does this calculation change if these individuals are in jobs with very high exposure (AKA, me). This is obviously a bit of a gray area in which reasonable experts can disagree, and disagree they did. The CDC panel voted 9-6 against recommending for this group but the CDC director added them to the group. You can see from the above how one could fall out on either side of the debate. The CDC director’s decision to go against the narrow majority decision of the advisory panel is not nearly as controversial as the news media made it sound. Imagine that, the media exaggerated and over-dramatized.
To me, the most strongest critique of giving booster shots is related to global health equity. Should we focus our efforts on getting a booster to those in wealthy countries before getting more vaccine doses to the rest of the world? This is more than just an ethical question. The Delta variant developed in India at a time where only 4% of the population was vaccinated. The next variant to cause us pain could be brewing in an underdeveloped unvaccinated population right now. If we delay getting these populations vaccinated it could come back to haunt us.
My Decision
When I was a kid, it was a common refrain for parents to tell their children to eat all the food because there were starving children in China. The thinking child would offer to package their excess vegetables and send them to China to help these poor children. This would obviously not work and highlights the tension between nationalism and globalism. I felt a twinge of guilt getting my booster but did so because I am highly exposed and the next variant may be worse and may get me early. The extra immune boost may help. I also did not think that my individual aliquot of vaccine would ever make it to an underdeveloped country just like my extra green beans wouldn’t help a starving child in China. The President has said that we can give boosters to our citizens and still vaccinate the rest of the world. I hope he is right.
What Should You do?
Since you are not likely a public policy maker, you are not likely going to allow geopolitical tension to impact your decision. I would recommend you get a booster if you fall into one of the groups defined by the CDC. If you are not in those groups, be thankful for your good health. While the booster may improve your immunity, you’ll be fine without it.
Daniel,
This was great, so informative.
Thank you, Lisa
LikeLike
Well done. The best article i ve seen about boosters. Say hi to your dad
Ron Fischler MD
LikeLike
I still wonder, after 16,000 death reports in VAERS, half within 48 hours of being vaccinated, the CDC has yet to issue any kind of autopsy report. One would expect at least a 1% sampling.
And I wonder why doctors aren’t asking the same question publicly. Do doctors really feel so badly threatened with repercussions they should speak out and question the vaccines?
LikeLiked by 1 person
You are mistaken in your understanding of how VAERS works. Your error come from a lack of understanding of the difference between assocuaand causation. I don’t have the time now to explain these issues but suggest you find unbiased sources to explain how they work.
LikeLike
Read my about page, then apologize.
It doesn’t require a medical school education to know that an autopsy is needed to determine cause of death.
German and Austrian pathologists have conducted autopsies on suspicious deaths post vaccination. But we have had no autopsy reports from the CDC, which might be alarming if anybody actually believed that the CDC was anything but a shill for pharma.
CDC: Cause of death? We doan need no steenkeeng cause of death.
LikeLiked by 1 person
This is blatantly false.
LikeLike
Your a wonderful asset answering all our questions!!! There are so many things in the news!! Great to hear whats Dr Grove advise!!!Thank you Dr Grove!😊
LikeLike
Let’s see. Not a single family member has succumbed to the virus from China. None of my friends have succumbed to the virus from China. A couple friends did mention family members, and I think they had other health problems, but I only hope the best for them. In our neighborhood, haven’t heard of one person succumbing to the virus. Two doctors, from two different hospitals, shared very few have come in with that virus, and almost all left well, except for their other health issues. Researching, we have discovered the stats are like other flus, actually better than some. **It’s all propaganda. It’s designed to control you, me, and everyone else, so we’re controlled and distracted while other things, more serious, are going on. Think for yourselves.
LikeLiked by 4 people
Is it possible that Israel’s statistics for breakthroughs are just commensurate with their amazing and comprehensive testing rates? Like a protective parent, a nation that cares fiercely about their peoples health exerts stronger surveillance and precaution.
LikeLike
I have personally seen dozens of people die from COVID with my own eyes. Their presentations are unique from other diseases and remarkably consistent. Have any of your friends worked in an ICU or are they just using their limited anecdotal exposures. You can’t make up 800,000 deaths. Thousands of doctors and nurses cannot all be lying about what they are seeing day in and day out. You CAN lie social media, however. The pandemic is very real and you are contributing to its spread.
LikeLike